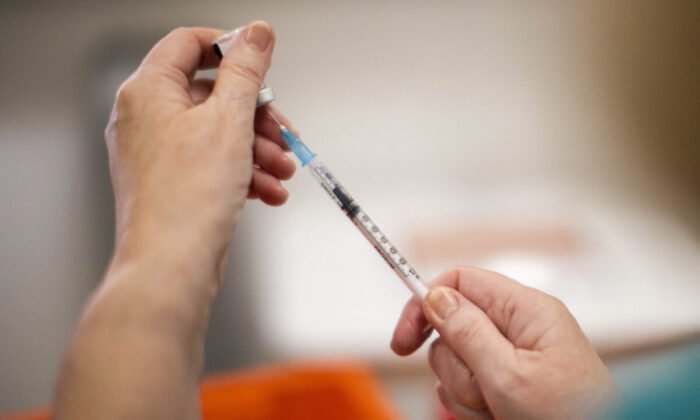
Public Was Kept Uninformed About Post COVID-19 Vaccination Myocarditis by Regulator for Four Months
The MHRA said it needed to assess data from multiple sources before adding warnings to COVID shots.
The UK Medicines and Healthcare Products Regulatory Agency (MHRA) detected a signal for post-vaccination myocarditis and pericarditis four months before telling the public, emails show.
In response, MRHA said that chose that time after it had “all available evidence, including that received from international regulators, rather than using any one source in isolation.”
Myocarditis or Pericarditis
A safety signal is information on a new or known adverse event that may be caused by a medicine and requires further investigation.
This was “following a thorough review of extremely rare reports of myocarditis and pericarditis after COVID-19 vaccination.”
“These events are extremely rare and tend to be mild when they do occur,” it said.
He was warned by Israel on Feb. 28, 2021, of around 40 post-vaccination cases of myocarditis, a form of heart inflammation, according to the emails.
On March 1, he wrote that “we are monitoring closely cases of myocarditis (triggered for Comirnaty as we have more reports) and already had a discussion with MRHA.”
It was claimed that the signal was a “chance finding.”
The emails were obtained through a freedom of information request by “Benedikt,” who was hospitalised on March 29, 2021, with myocarditis after receiving his second Pfizer COVID-19 vaccination.
Benedikt, a consultant, asked that his last name not be used due to a fear of professional repercussions.
One Source in Isolation
MHRA indicated it did detect a signal, but it needed to assess data from multiple sources.
“Myocarditis was one of a number of adverse events of special interest that the MHRA and other global regulators have monitored since the start of C-19 vaccinations in line with our COVID-19 surveillance strategy,” the MHRA told The Epoch Times in an email.
“This included monitoring of Yellow Card data reported to the MHRA, data recorded in electronic health care records and evidence generated through independent studies,” it said.
“With any such regular repeated analysis, there is an increased possibility of chance findings which do not reflect true associations, and therefore, it is important that data from multiple sources are assessed,” it
Source link